Shockwave Therapy in Victoria BC
We are offering Shockwave Therapy Treatments at our main Victoria Physiotherapy Clinic located at 3200 Shelbourne Street #100B, Victoria, B.C., V8P 5G8. The clinic is conveniently located near the Hillside Mall at the corner of North Dairy and Shelbourne Street. We also offer Shockwave Therapy at our Cook Street Clinic located at 1175 Cook Street #308, Victoria, B.C. 250-381-9828.
To book an appointment for Shockwave Therapy please call our clinic today at 250-598-9828 or book online.
 What Conditions Can Be Treated in Victoria BC with Shockwave Therapy?
What Conditions Can Be Treated in Victoria BC with Shockwave Therapy?
Shockwave Therapy can be used to treat a wide variety of musculoskeletal conditions, in particular, those involving areas where major connective tissue attaches to bone. Common sites that can be successfully treated are:
- Foot – Plantar Fasciitis, heel spurs & Achilles tendonitis
- Knee – Patellar tendonitis, jumper's knee & shin pain
- Elbow – tennis or golfer’s elbow
- Shoulder – rotator cuff tendonitis & calcification
- Hip – trochanteric bursitis
- Muscles – various trigger points throughout the body and muscle tension
- Bones-Stress fractures, non union's(delayed bone healing)
- Nerves-Morton's Neuroma
 What are the Advantages of Shockwave Therapy (ESWT)?
What are the Advantages of Shockwave Therapy (ESWT)?
Shockwave therapy is a recent development that is used successfully by healthcare providers that specialize in musculoskeletal disorders. As compared to other treatment methods, the advantages are:
- Quickly reduces pain
- No medication is needed
- Avoids surgery and anasthesia
- No side effects
- No risk of allergies
- Accelerates healing
- Effective for chronic conditions
 What are the Medical Effects of Shockwave Therapy?
What are the Medical Effects of Shockwave Therapy?
The acoustic waves used in Shockwave therapy interact with your tissues causing the overall medical effects of accelerated tissue repair and cell growth, analgesia and mobility restoration.
- New Blood Vessel Formation
- Reversal of Chronic Inflammation
- Stimulation of Collagen Production
- Dissolution of Calcified Fibroblasts
- Dispersion of Pain Mediator "Substance P"
- Release of Trigger Points
 How does Shockwave Therapy work?
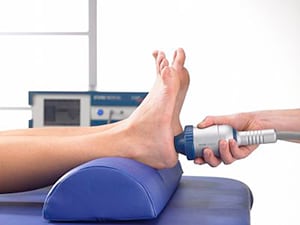
How does Shockwave Therapy work?
Shockwaves accelerate the healing process by activating the body’s self-healing powers, particularly in cases where the body has been unable to do it on its own. It stimulates metabolism and enhances blood circulation which enables damaged tissue to regenerate and eventually heal. The treatment relieves pain by producing an analgesic effect on the treatment area. Healing occurs over several treatments by initiating an inflammatory response and ultimately vascularization to the area. Shockwave therapy accelerates the healing process in the body by stimulating the metabolism and enhancing blood circulation to regenerate and heal damaged tissue. Strong energy pulses are applied with our equipment to the affected area. These pulses occur for very short periods of time, creating micro-cavitation bubbles that expand and burst. The force created by these bubbles penetrates tissue and stimulates cells in the body that are responsible for bone and connective tissue healing. In many instances, shockwave therapy is most effective in cases where the human body has been unable to heal itself on its own. These high energy acoustic waves that are transmitted through the surface of the skin are spread radially (spherically) into the body and the body responds with increased metabolic activity around the area of the pain. This stimulates and accelerates the healing process and is especially useful for those suffering from chronic heel, shoulder, knee, achilles, elbow and back pain. The use of shockwave in therapy is that it effectively takes a tissue from a more chronic to a more acute state, and in doing so, provides a stimulus (trigger) to a 'stalled' repair sequence".
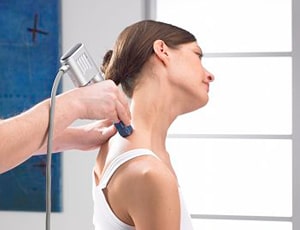
Your Victoria Shelbourne Physiotherapist will apply shockwaves through a specially designed hand piece that produces strong energy pulses for short periods of time. The shockwave energy pulses are applied directly to the affected tissue areas in controlled procedure.Shockwaves have a mechanical effect on the tissue. Pressure in the front of the shockwave is transmitted into the tissue, creating micro-cavitation bubbles that expand and burst into a resultant force. This force penetrates tissue and stimulates cells in the body which are responsible for bone (osteoblast) and connective tissue (fibroblast) healing. Extracorporeal Shockwave Therapy (known as ESWT) is a modern and highly effective treatment method validated by research. The process introduces high-energy sound waves into the painful areas of the body. and with this innovative therapy approach, pathological alterations of tendons, ligaments, capsules, muscles and bones can be eliminated systematically.
Research has also shown that Shockwave also breaks down calcium deposits.
 What is the success rate of Shockwave Therapy?
What is the success rate of Shockwave Therapy?
After only 2-3 sessions, over 80% of patients report a significant reduction in pain.
- 90% improvement for plantar fasciitis (Journal of Orthopedic Research, 2005)
- 91% improvement for calcific tendonitis (Journal of American Medical Association, 2003)
- 77% improvement for tennis elbow (Journal of Orthopedics, 2005)
How Long Does Shockwave Therapy Treatment Last?
The therapy session takes about 10-15 minutes depending on the disorder that is treated. In general, 3-5 sessions are necessary at weekly intervals.
Ask your doctor or therapist if your condition can be treated by Shockwave Therapy and book your treatment sessions today at Shelbourne Physiotherapy in Victoria BC!
Shockwave Therapy Research Articles
The following articles confirm the scientific validity of Shockwave Therapy;
ESWT is a force to be reckoned with
Extracorporeal Shock Wave Therapy compared with Surgery for Hypertrophic Long Bone Nonunions
How Shockwave Therapy helps heal Sports and Overuse Injuries
High Energy Extracorporeal Shockwave Therapy as a Treatment for Insertional Achilles Tendinopathy
Extracorporeal Shockwave for Chronic Patellar Tendinopathy
Low Energy Extracorporeal Shockwave Therapy as a treatment for Medial Tibial Stress Syndrome
Extracorporeal Shockwave Therapy in Musculoskeletal Disorders
Physical Therapy- Effectiveness of Radial Shockwave Therapy for Calcific Tendinitis of the Shoulder
Biological Mechanism of Musculoskeletal Shockwaves
Current Knowledge on evidence based shockwave treatments for shoulder pathology
Radial Shockwave Therapy in Calcific Tendonitis of the Rotator Cuff
Safety and Efficacy of ESWT for Chronic Lateral Epicondylitis
ESWT for the Treatment of Plantar Fascitis
Shockwave Therapy for Patients with Lateral Epicondylitis of the Elbow
Radial Extracorporeal Shockwave Therapy (rESWT) in Chronic Plantar Heel Pain
Radial Shockwave Therapy in Heel Spur (Plantar Fasciitis)
Shockwave Therapy for Treatment of Foot and Ankle Conditions
ESWT for Plantar fascitis: What do the Long-Term Results Reveal?
Shockwaves fired into my Foot cured my crippling pain and got me back into heels
Extracorporeal Shockwave Therapy without Local Anasthesia for Chronic Lateral Epicondylitis
Frequently Asked Questions for ESWT
Calcific Tendinitis of the Rotator Cuff
Lateral Epicondylitis of the Elbow
Extracorporeal Shockwave Therapy for the Treatment of Chronic Pelvic Pain Syndrome in Males
Lateral Epicondylitis Treatment
Shockwave Therapy in Chronic Achiles Tendinopathy
Calcific Tendonitis of the Shoulder Girdle-Shockwave Treatment
More Shockwave Victoria BC Abstract Articles
Acute-Phase RSWT in Elite Football
Low-Energy Extracorporeal Shock Wave Therapy as a Treatment for Greater Trochanteric Pain Syndrome
Revolutionary medical treatment comes to Surrey
A neural model for chronic pain and pain relief by extracorporeal shock wave treatment
Extracorporeal shockwave lithotripsy for calcific tendonitis (tendinopathy) of the shoulder
Radial Shock Wave Therapy in Calcifying tendinitis of the Rotator Cuff – A Prospective Study
Treatment of Painful Heel with Shockwave Therapy
Pain relief by extracorporeal shockwave therapy: an update on the current understanding
Treatment for Osteonecrosis of the Femoral Head
Comparison of Extracorporal Shock Waves with Core Decompression and Bone-Grafting
Shock Wave Therapy for Patients with Lateral Epicondylitis of the Elbow
Extracorporeal Shock Wave Therapy (ESWT) in Orthopaedics and Traumatology
Extracorporal Shock Wave Therapy in the Treatment of Chronic Tendinopathies
ESWT in the Treatment of Calcific Tendinitis of the Rotator Cuff
Abstracts ISMST 10th International ISMST Congress Toronto 2007
ESWT of myofascial trigger points, 2003-2008
Effectiveness of Radial Shock-Wave Therapy for Calcific Tendinitis of the Shoulder
Extracorporeal shock wave lithotripsy for calcific tendonitis (tendinopathy) of the shoulder
Comparison of radial shockwaves and conventional physiotherapy for treating plantar fasciitis
Low-energy extracorporeal shock wave as a treatment for medial tibial stress syndrome
Current understanding of pain relief by extracorporeal shockwave therapy (ESWT)
Extracoroporeal Shockwave Therapy for Refractory Plantar Fascitis
Lateral epicondylitis: This is still a main indication for extracorporeal shockwave therapy
Radial extracorporeal shockwave therapy for the treatment of finger tenosynovitis (trigger digit)
Arthroscopy surgery versus shock wave therapy for chronic calcifying tendinitis of the shoulder
Effects of Shockwave Therapy on glycosaminoglycan expression during bone healing
Radial extracorporeal pressure pulse therapy for the primary long bicipital tenosynovitis a prospective randomized controlled study.
Liu S, Zhai L, Shi Z, Jing R, Zhao B, Xing G.
Source
Orthopaedic Department, Medical College Affiliated Hospital of Chinese People's Armed Police Force, Tianjin, China.
Abstract
Long bicipital tenosynovitis is regarded as one of the common causes of shoulder pain and dysfunction. The traditional therapeutic approach includes a variety of conservative treatments, but these treatments are not substantiated, owing to the lack of proven clinical efficacy. Radial extracorporeal shock wave therapy (rESWT) uses a pneumatically generated and radially propagating low-energy pressure pulse and has been clinically shown to be a new alternative form of treating refractory soft tissue inflammation. While treating patients suffering from long bicipital tenosynovitis, a randomized, controlled trial was conducted to analyze the effects of radial shock wave therapy on pain and function. Seventy-nine adults with long bicipital tenosynovitis were randomized to receive either active (1500 pulses, 8 Hz, 3 bars) or sham treatment through four sessions that were held once a week. All of these adults were assessed before treatment and at time intervals of 1, 3 and 12 months since the completion of the treatment. The outcomes were measured through the visual analogue scale (VAS) and L'Insalata shoulder questionnaire. Mean VAS in the rESWT group showed significant and sustained reduction from 5.67 ± 1.32 at baseline to 2.58 ± 1.49 at one month, 1.83 ± 1.25 at three months and 1.43 ± 0.94 at 12 months from baseline, whereas the sham group's mean VAS was 6.04 ± 0.97 before treatment and stabilized at 5.57 ± 0.84 at 12 months. Similar trends were found for the function scores. Mean scores were increased after rESWT from 60.57 ± 6.91 at baseline to 79.85 ± 6.59 at 1 month and 83.44 ± 5.21 at 12 months from baseline. Both pain and function scores showed significant differences between the two groups (p < 0.001). The rESWT group consisted of "invalid conservative treatment subgroup" and "none conservative treatment subgroup." Both groups showed good recovery and prognosis. Therefore, we recommend rESWT in treating primary long bicipital tenosynovitis.
Extracorporeal shockwave therapy in musculoskeletal disorders.
Wang CJ.
Source
Department of Orthopedic Surgery, Kaohsiung Chang Gung Memorial Hospital, Kaohsiung City, Taiwan. w281211@adm.cgmh.com.tw
Abstract
The sources of shockwave generation include electrohydraulic, electromagnetic and piezoelectric principles. Electrohydraulic shockwaves are high-energy acoustic waves generated under water explosion with high voltage electrode. Shockwave in urology (lithotripsy) is primarily used to disintegrate urolithiasis, whereas shockwave in orthopedics (orthotripsy) is not used to disintegrate tissues, rather to induce tissue repair and regeneration. The application of extracorporeal shockwave therapy (ESWT) in musculoskeletal disorders has been around for more than a decade and is primarily used in the treatment of sports related over-use tendinopathies such as proximal plantar fasciitis of the heel, lateral epicondylitis of the elbow, calcific or non-calcific tendonitis of the shoulder and patellar tendinopathy etc. The success rate ranged from 65% to 91%, and the complications were low and negligible. ESWT is also utilized in the treatment of non-union of long bone fracture, avascular necrosis of femoral head, chronic diabetic and non-diabetic ulcers and ischemic heart disease. The vast majority of the published papers showed positive and beneficial effects. FDA (USA) first approved ESWT for the treatment of proximal plantar fasciitis in 2000 and lateral epicondylitis in 2002. ESWT is a novel non-invasive therapeutic modality without surgery or surgical risks, and the clinical application of ESWT steadily increases over the years. This article reviews the current status of ESWT in musculoskeletal disorders.
Extracorporeal shock wave therapy for plantar fasciitis.
Perez M, Weiner R, Gilley JC.
Source
Clintonville Foot and Ankle Group, Inc., 3695 N. High Street, Columbus, OH 43214, USA.
Abstract
Shock wave therapy is quickly becoming a mainstay treatment for chronic recalcitrant plantar fasciitis, and many more applications for this therapy may exist. Many advances have been made in regard to this modality of treatment in just a few decades since it was first investigated in the 1950s. Much research has been conducted, revealing the physics and physiologic effect of shock wave therapy. Devices are now approved that produce shock waves for medicinal purposes by one of the three primary methods of shock wave generation. Studies and research are actively being reported and published that demonstrate shock wave therapy success rates comparable to those found in surgical intervention but without the risks inherent in surgery. In conclusion, ESWT has proved to be a viable treatment option for the intervention of chronic recalcitrant plantar fasciitis.
Randomized, placebo-controlled, double-blind clinical trial evaluating the treatment of plantar fasciitis with an extracoporeal shockwave therapy (ESWT) device: a North American confirmatory study.
Kudo P, Dainty K, Clarfield M, Coughlin L, Lavoie P, Lebrun C.
Source
Fowler Kennedy Sport Medicine Clinic, 3M Centre University of Western Ontario, London, Ontario N6A 3K7, Canada.
Abstract
Despite numerous publications and clinical trials, the results of treatment of recalcitrant chronic plantar fasciitis with extracorporeal shockwave therapy (ESWT) still remain equivocal as to whether or not this treatment provides relief from the pain associated with this condition. The objective of this study was to determine whether extracorporeal shock wave therapy can safely and effectively relieve the pain associated with chronic plantar fasciitis compared to placebo treatment, as demonstrated by pain with walking in the morning. This was set in a multicenter, randomized, placebo-controlled, double-blind, confirmatory clinical study undertaken in four outpatient orthopedic clinics. The patients, 114 adult subjects with chronic plantar fasciitis, recalcitrant to conservative therapies for at least 6 months, were randomized to two groups. Treatment consisted of approximately 3,800 total shock waves (+/-10) reaching an approximated total energy delivery of 1,300 mJ/mm(2) (ED+) in a single session versus placebo treatment. This study demonstrated a statistically significant difference between treatment groups in the change from baseline to 3 months in the primary efficacy outcome of pain during the first few minutes of walking measured by a visual analog scale. There was also a statistically significant difference between treatments in the number of participants whose changes in Visual Analog Scale scores met the study definition of success at both 6 weeks and 3 months posttreatment; and between treatment groups in the change from baseline to 3 months posttreatment in the Roles and Maudsley Score. The results of this study confirm that ESWT administered with the Dornier Epos Ultra is a safe and effective treatment for recalcitrant plantar fasciitis.
Radial extracorporeal shock wave therapy is safe and effective in the treatment of chronic recalcitrant plantar fasciitis: results of a confirmatory randomized placebo-controlled multicenter study.
Gerdesmeyer L, Frey C, Vester J, Maier M, Weil L Jr, Weil L Sr, Russlies M, Stienstra J, Scurran B, Fedder K, Diehl P, Lohrer H, Henne M, Gollwitzer H.
Source
Department of Orthopedic and Traumatology, Technical University Munich, Klinikum Rechts der Isar, Germany. Gerdesmeyer@aol.com
Abstract
BACKGROUND:
Radial extracorporeal shock wave therapy is an effective treatment for chronic plantar fasciitis that can be administered to outpatients without anesthesia but has not yet been evaluated in controlled trials.
HYPOTHESIS:
There is no difference in effectiveness between radial extracorporeal shock wave therapy and placebo in the treatment of chronic plantar fasciitis.
STUDY DESIGN:
Randomized, controlled trial; Level of evidence, 1.
METHODS:
Three interventions of radial extracorporeal shock wave therapy (0.16 mJ/mm(2); 2000 impulses) compared with placebo were studied in 245 patients with chronic plantar fasciitis. Primary endpoints were changes in visual analog scale composite score from baseline to 12 weeks' follow-up, overall success rates, and success rates of the single visual analog scale scores (heel pain at first steps in the morning, during daily activities, during standardized pressure force). Secondary endpoints were single changes in visual analog scale scores, success rates, Roles and Maudsley score, SF-36, and patients' and investigators' global judgment of effectiveness 12 weeks and 12 months after extracorporeal shock wave therapy.
RESULTS:
Radial extracorporeal shock wave therapy proved significantly superior to placebo with a reduction of the visual analog scale composite score of 72.1% compared with 44.7% (P = .0220), and an overall success rate of 61.0% compared with 42.2% in the placebo group (P = .0020) at 12 weeks. Superiority was even more pronounced at 12 months, and all secondary outcome measures supported radial extracorporeal shock wave therapy to be significantly superior to placebo (P < .025, 1-sided). No relevant side effects were observed.
CONCLUSION:
Radial extracorporeal shock wave therapy significantly improves pain, function, and quality of life compared with placebo in patients with recalcitrant plantar fasciitis.
Clin Rheumatol. 2012 May;31(5):807-12. Epub 2012 Jan 27.
Physical therapy, corticosteroid injection, and extracorporeal shock wave treatment in lateral epicondylitis. Clinical and ultrasonographical comparison.
Source
Physical Medicine and Rehabilitation Clinic, Ankara Training and Research Hospital, Ankara, Turkey.
Abstract
The aim of this study was to compare--clinically and ultrasonographically--the therapeutic effects of physical therapy modalities (hot pack, ultrasound therapy, and friction massage), local corticosteroid injection, and extracorporeal shock wave treatment (ESWT) in lateral epicondylitis (LE). Fifty-nine elbows of 59 patients with LE were randomized into three treatment groups receiving either physical therapy, a single corticosteroid injection, or ESWT. Visual analogue scale (VAS) was used to assess pain intensity, Jamar hydraulic dynamometer for grip strength, finger dynamometer for pinch strength (before treatment, on the first, third, and sixth months of treatment). All subjects were also evaluated with ultrasonography before and 6 months after treatment. In all groups, VAS scores of the patients were found to decrease significantly on the first, third, and sixth months of treatment. With respect to grip strength evaluations, the increase after treatment was significant only on the first month in group II; on the first and third months in group I; and on the first, third, and sixth months of treatment in group III. Pinch strength and ultrasonographical findings did not change during follow-up in any group. We imply that physical therapy modalities, corticosteroid injection, and ESWT have favorable effects on pain and grip strength in the early period of LE treatment. The increase in grip strength lasts longer with ESWT. On the other hand, ultrasonographic findings do not change in the first six months of these treatment methods.
Shockwave Therapy for Calcium Deposits in Shoulder
Reference:Adnan Saithna, BMedSci(Hons), MBChB, MRCSEd, et al.
Is Extracorporeal Shockwave Therapy for Calcifying Tendinitis of the Rotator Cuff Associated with a Significant Improvement in the Constant-Murley Score? A Systematic Review.
In Current Orthopaedic Practice. September/October 2009. Vol. 20. No. 5. Pp. 566-571.
What's the best way to treat calcifying tendinitis of the shoulder that doesn't respond to physical therapy, medications, or steroid injections? The authors of this systematic review report that the use of extracorporeal shockwave therapy (ESWT) has proven successful, though we still don't know if it is the best treatment approach. That remains to be determined in future studies.
What is calcifying or calcific tendinitis? It's a degenerative condition affecting the four tendons surrounding the shoulder called the rotator cuff. These include the supraspinatus, infraspinatus, teres minor, and subscapularis muscles. All four muscles can be affected, but usually it's just one of the four. And the tendons are listed here in declining order of frequency (i.e., supraspinatus is affected most often and subscapularis least often).
Calcium crystals called calcium pyrophosphate are deposited in the tendons. No one knows where these crystals come from exactly. But once the tendons start to degenerate, the crystals are released into the soft tissues as the tendon fibrils break down. Research shows that the calcium crystals help the tendon degenerate. The tendons harden and symptoms of impingement can develop. With impingement, there is shoulder pain when the arm is raised overhead or to the side above shoulder level. The stiff tendon doesn't move and glide as it should and it gets pinched between the bony structures of the shoulder. Sometimes the person with this problem can move the arm through the pain all the way overhead. But other people have limited motion that leads to decreased function.
By sorting through five years of data from recently published studies, researchers from the Department of Trauma and Orthopaedic Surgery in England were able to confirm that all studies showed improvement after treating calcifying tendinitis of the rotator cuff with extracorporeal shockwave therapy (ESWT). ESWT is the use of sound waves to create enough energy to disintegrate the calcium deposits. It has been used with good results for other problems like gallstones and kidney stones. Once the calcium crystals have been broken up, it appears that the body absorbs them because X-rays show they disappear.
Most of the studies included patients with Types I and II calcification. There are three types of calcifying tendinitis diagnosed by X-rays. Type I has deposits that have clear outlines. A line can be drawn around the dense deposits to show exactly where they are, their size, and their shape. Type II disease has a clear outline but tends to be spread out more through the tissue and harder to see as a distinct shape. Type III lesions look cloudy without a specific form, shape, or outline.
All studies used a scoring system called the Constant-Murley score to measure results before and after treatment. Having one test used by everyone made it possible to compare the outcomes from one study to the next -- even when the studies weren't all conducted exactly the same way. The authors point out that this advantage was also a disadvantage. With only one measure of results was used, it's impossible to know if other test measures might have shown a different result (better or worse). They suggest that future studies use other scoring systems for a comparison.
But for now, it looks like extracorporeal shockwave therapy is safe and effective for this potentially disabling condition. Significant improvement in motion, pain, strength, and function was consistently reported in all studies included in the review. Improvements were reported using both high-energy and low-energy shockwave therapy but high-energy had the best results. Low-energy therapy was better than no treatment or sham (placebo) groups.
Low-Energy Extracorporeal Shock Wave Therapy as a Treatment for Greater Trochanteric Pain Syndrome
The American Journal of Sports Medicine, Vol. X, No. X
John P. Furia, MD, Jan D. Rompe, MD, and Nicola Maffulli, MD, MS, PhD, FRCS (Orth), FFSEM (UK)From SUN Orthopedics and Sports Medicine, Lewisburg, Pennsylvania, OrthoTrauma Evaluation Center, Mainz, Germany, Centre for Sports and Exercise, Barts and the London School of Medicine and Dentistry, London, United Kingdom
Background: Greater trochanteric pain syndrome is often a manifestation of underlying gluteal tendinopathy. Extracorporeal shock wave therapy is effective in numerous types of tendinopathies.
Hypothesis: Shock wave therapy is an effective treatment for chronic greater trochanteric pain syndrome.
Study Design: Case control study; Level of evidence, 3.
Methods: Thirty-three patients with chronic greater trochanteric pain syndrome received low-energy shock wave therapy (2000 shocks; 4 bars of pressure, equal to 0.18 mJ/mm2; total energy flux density, 360 mJ/mm2). Thirty-three patients with chronic greater trochanteric pain syndrome were not treated with shock wave therapy but received additional forms of nonoperative therapy (control). All shock wave therapy procedures were performed without anesthesia. Evaluation was by change in visual analog score, Harris hip score, and Roles and Maudsley score.
Results: Mean pretreatment visual analog scores for the control and shock wave therapy groups were 8.5 and 8.5, respectively. One, 3, and 12 months after treatment, the mean visual analog score for the control and shock wave therapy groups were 7.6 and 5.1 (P < .001), 7 and 3.7 (P < .001), and 6.3 and 2.7 (P < .001), respectively. One, 3, and 12 months after treatment, mean Harris hip scores for the control and shock wave therapy groups were 54.4 and 69.8 (P < .001), 56.9 and 74.8 (P < .001), and 57.6 and 79.9 (P < .001), respectively. At final follow-up, the number of excellent, good, fair, and poor results for the shock wave therapy and control groups were 10 and 0 (P < .001), 16 and 12 (P < .001), 4 and 13 (P < .001), and 3 and 8 (P < .001), respectively. Chi-square analysis showed the percentage of patients with excellent (1) or good (2) Roles and Maudsley scores (ie, successful results) 12 months after treatment was statistically greater in the shock wave therapy than in the control group (P < .001).
Conclusion: Shock wave therapy is an effective treatment for greater trochanteric pain syndrome.
Keywords: extracorporeal shock wave therapy; hip; subgluteus bursa; bursitis
Evidence to Support Shock Wave Therapy for Plantar Fasciitis
Plantar Fascitis is a painful condition affecting the bottom of the foot. It is a common cause of heel pain and is sometimes called a heel spur. Plantar fasciitis is the correct term to use when there is active inflammation. Acute plantar fasciitis is defined as inflammation of the origin of the plantar fascia and fascial structures around the area. Plantar fasciitis is usually just on one side. In about 30 per cent of all cases, both feet are affected.
Treatment is usually with conservative (nonoperative) care. This could include stretching, wearing a splint at night, the use of antiinflammatory medications, and/or a special arch support to help reduce the pressure on the fascia.
Shock wave therapy is a newer form of nonsurgical treatment. It uses a machine to generate shock wave pulses to the sore area. Patients generally receive the treatment once each week for up to three weeks. It is not known exactly why it works for plantar fasciitis. It's possible that the shock waves disrupt the plantar fascial tissue enough to start a healing response. The resulting release of local growth factors and stem cells causes an increase in blood flow to the area. Recent studies indicate that this form of treatment can help ease pain, while improving range of motion and function.
There are different types of shock wave therapy. In this study, researchers from Taiwan conduct a systematic review and meta-analysis comparing the effectiveness of two major types of shock wave therapy. The most common type is called focused shock wave therapy (FSW). A newer, alternative form called radial shock wave therapy (RSW) was also evaluated.
Focused shock wave (FSW) therapy is just as it sounds: the energy wave is directed at a specific area. FSW concentrates the wave field whereas radial shock wave (RSW) disperses the energy over a wider range. With RSW, it is not necessary to find the painful spots before applying the energy wave.
A particular area of interest in this study was to see the value in using different intensity levels, which represent energy flow through the tissue. Turning the intensity up may provide more pain relief but could also temporarily increase pain, local swelling, and tenderness. Studies have not been done to determine the most optimal intensity to use when treating plantar fasciitis with shock wave therapy.
Focus shock wave therapy can be delivered in three intensities: low, medium, and high. Patients receiving FSW were divided into three groups based on the intensity of wave delivery. Patients receiving RSW made up the fourth group. Results were measured based on pain reduction and overall success of the treatment. The goal was to see if one type of shock therapy was superior to the others in treating plantar fasciitis.
What did they find? Well, first of all, any type of shock wave therapy yielded better results than a "sham" or placebo (pretend) treatment. The best results were gained using radial shock wave (RSW) therapy. Focused shock wave (FSW) gave the best results when used at the highest energy density tolerated by the patient in the medium intensity range.
For those who use this modality to treat plantar fasciitis, the authors say don't go out and purchase a radial shock wave machine if you already have a focused shock wave device. Anyone just considering purchasing this equipment is advised to select radial shock wave therapy. It costs less and gives better results with fewer potential side effects.
Reference:
Ke-Vin Chang, MD, et al. Comparative Effectiveness of Focused Shock Wave Therapy of Different Intensity Levels and Radial Shock Wave Therapy for Treating Plantar Fasciitis: A Systematic Review and Network Meta-Analysis. In The American Journal of Sports Medicine. July 2012. Vol. 93. No. 7. Pp. 1259-1268.
Extracorporeal shock wave therapy without local anesthesia for chronic lateral epicondylitis
J Bone Joint Surg AM, 2005 Jun:87(6):1297-304
Pettrone FA, McCall BR.
Source
Commonwealth Orthopaedics, 1635 North George Mason Drive, Suite 310, Arlington, VA 22205, USA.
Abstract
BACKGROUND:
The use of extracorporeal shock wave therapy for the treatment of lateral epicondylitis is controversial. The purpose of this study was to evaluate the use of extracorporeal shock wave therapy without local anesthesia to treat chronic lateral epicondylitis.
METHODS:
One hundred and fourteen patients with a minimum six-month history of lateral epicondylitis that was unresponsive to conventional therapy were randomized into double-blind active treatment and placebo groups. The protocol consisted of three weekly treatments of either low-dose shock wave therapy without anesthetic or a sham treatment. Patients had a physical examination, including provocation testing and dynamometry, at one, four, eight, and twelve weeks and at six and twelve months after treatment. Radiographs, laboratory studies, and electrocardiograms were also evaluated prior to participation and at twelve weeks. A visual analog scale was used to evaluate pain, and an upper extremity functional scale was used to assess function. Crossover to active treatment was initiated for nonresponsive patients who had received the placebo and met the inclusion criteria after twelve weeks.
RESULTS:
A total of 108 of the 114 randomized patients completed all treatments and the twelve weeks of follow-up required by the protocol. Sixty-one patients completed one year of follow-up, whereas thirty-four patients crossed over to receive active treatment. A significant difference (p = 0.001) in pain reduction was observed at twelve weeks in the intent-to-treat cohort, with an improvement in the pain score of at least 50% seen in 61% (thirty-four) of the fifty-six patients in the active treatment group who were treated according to protocol compared with 29% (seventeen) of the fifty-eight subjects in the placebo group. This improvement persisted in those followed to one year. Functional activity scores, activity-specific evaluation, and the overall impression of the disease state all showed significant improvement as well (p < 0.05). Crossover patients also showed significant improvement after twelve weeks of active treatment, with 56% (nineteen of thirty-four) achieving an improvement in the pain score of at least 50% (p < 0.0001).
CONCLUSIONS:
These results demonstrate that low-dose shock wave therapy without anesthetic is a safe and effective treatment for chronic lateral epicondylitis.
Repetitive low-energy shock wave application without local anesthesia is more efficient than repetitive low-energy shock wave application with local anesthesia in the treatment of chronic plantar fasciitis
Rompe JD, Meurer A, Nafe B, Hofmann A, Gerdesmeyer L.
Background:
It remains unclear whether application of local anesthesia (LA) interferes with clinical efficacy of extracorporeal shock wave therapy (ESWT) for chronic plantar fasciitis.
Aims: To evaluate the effect of local anesthesia on the clinical outcome after repetitive low-energy ESWT for chronic plantar fasciitis.
Methods:
Eighty-six patients with chronic plantar fasciitis were randomly assigned to receive either low-energy ESWT without LA, given weekly for three weeks (Group I, n=45; 3 x 2000 pulses, total energy flux density per shock 0.09 mJ/mm2) or identical ESWT with LA (Group II, n=41). Primary outcome measure was: Reduction of pain from baseline to month 3 post-treatment in a pain numeric rating scale [0-10 points] during first steps in the morning, evaluated by an independent blinded observer. Calculations were based on intention-to-treat.
Results:
No difference was found between the groups at baseline. At 3 months, the average pain score was 2.2+/-2.0 points for patients of Group I, and 4.1+/-1.5 points for patients of Group II. The mean between-group difference was 1.9 points (95% CI: [1.1-2.7 points]; P<.001). Significantly more patients of Group I achieved 50% reduction of pain compared to Group II (67% vs 29%, P<.001).
Conclusions: ESWT as applied should be done without LA in patients suffering from chronic heel pain. LA applied prior treatment reduced the efficiency of low-energy ESWT.
Arch Phys Med Rehabil. 2013 Mar 13. pii: S0003-9993(13)00205-0. doi: 10.1016/j.apmr.2013.01.030. [Epub ahead of print]
Clinical improvement and resorption of calcifications in calcific tendinitis of the shoulder after shock wave therapy at 6 months follow-up. A systematic review and meta-analysis.
Ioppolo F, Tattoli M, Di Sante L, Venditto T, Tognolo L, Delicata M, Rizzo RS, Di Tanna G, Valter S.
Source: Physical Medicine and Rehabilitation Unit, Azienda Policlinico Umberto I, Rome, Italy. Electronic address: francescoioppolo@yahoo.it.
Abstract
OBJECTIVE: To evaluate the effect of the Shock wave therapy (SWT) on functional improvements and reduction of pain, and what is rate of disappearance of calcifications after therapy at 6 month follow up.
DATA SOURCES: Articles were searched from the COCHRANE LIBRARY, MEDLINE, EMBASE, CINAHL and OVID DATABASE.
STUDY SELECTION:We included randomized controlled trials from 1992 to 2011 and their quality was assessed using the PEDro scale.
DATA EXTRACTION: Studies were evaluated by two independent reviewers for their methodological quality. If disagreement arose the plan was that it would be settled by a third reviewer. Then data were extracted and cross-checked for accuracy. The reviewers were not blinded to the authors of the articles.
DATA SYNTHESIS: In studies of Hearnden, Hsu, Cacchio and Cosentino the resorption of calcifications was evaluate using meta-analysis because in them there were two groups of treatment, while the studies of Peters and Gerdesmeyer were analyzed descriptively because they considered three groups of treatment. Fixed and random effects models were used to meta-analyze total and partial resorption ratios and to assess heterogeneity the I2 statistics were calculated.
CONCLUSIONS: We found a clinical improvement with a pooled Total Resorption Ratio of 27.19 (95% CI: 7.20-102.67) and a pooled Partial Resorption Ratio of 16.22 (95% CI: 3.33-79.01). SWT increases shoulder function, reduces pain, and it is effective in dissolving calcifications. These results were maintained over the following 6 months.
Am J Phys Med Rehabil. 2013 Apr 2.
Effectiveness of Extracorporeal Shock Wave Therapy in Chronic Plantar Fasciitis: A Meta-analysis.
Source: Dizon JN, Gonzalez-Suarez C, Zamora MT, Gambito ED.
From the Department of Physical Medicine and Rehabilitation, University of Santo Tomas Hospital, Manila, Philippines.
Abstract
The objective of this study was to evaluate the effectiveness of extracorporeal shock wave therapy (ESWT) in treating chronic plantar fasciitis. An online database search was conducted for studies using ESWT in managing chronic plantar fasciitis. Eleven high-quality randomized controlled trials were included in the meta-analysis and showed that ESWT was more effective in reducing morning pain (weighted mean difference, -0.77 [95% confidence interval {CI}, -1.30 to -0.25]; odds ratio, 0.65 [95% CI, 0.42-1.00]). Moderate-intensity ESWT was more effective in decreasing overall and activity pain (weighted mean difference, -6.6 [95% CI, -6.74 to -6.46], and weighted mean difference, 0.47 (95% CI, 0.30-0.74). Both moderate- and high-intensity ESWT were more effective in improving functional outcome, with odds ratios of 0.51 (95% CI, 0.30-0.84) and 0.47 (95% CI, 0.29-0.75). The adverse effects that were seen more in ESWT were pain on the calcaneal area and calcaneal erythema. This study concludes that moderate- and high-intensity ESWT were effective in the treatment of chronic plantar fasciitis.
Radial extracorporeal shock wave therapy improves recalcitrant plantar fasciitis symptoms.
OrthoEvidence Advanced Clinical Evidence Report. In: Ortho Evidence. Created Oct 01, 2011. Last modified Oct 01, 2012. Retrieved Jul 26, 2013 from http://www.myorthoevidence.com/?section=15&id=2807.
Radial Extracorporeal Shock Wave Therapy Is Safe and Effective in the Treatment of Chronic Recalcitrant Plantar Fasciitis
Results of a Confirmatory Randomized Placebo-Controlled Multicenter Study
Ludger Gerdesmeyer,MD, PhD, Carol Frey, MD, Johannes Vester, PhD,Markus Maier, PhD, Lowell Weil Jr, DPM, Lowell Weil Sr,DPM, Martin Russlies, PhD,John Stienstra,DPM, Barry Scurran, DPM, Keith Fedder, MD, Peter Diehl, MD,Heinz Lohrer, MD, Mark Henne, MD, and Hans Gollwitzer, MDFrom the Department of Orthopedic and Traumatology, Technical University Munich, KlinikumRechts der Isar, Germany, the Department of Joint Arthroplasty and Clinical Science, MareClinic, Kiel, Germany, Orthopaedic Foot and Ankle Center, Manhattan Beach, California, DVData Analyses and Study Planning, Biometrics in Medicine, Gauting, Germany, the Departmentof Orthopedics, Ludwig Maximilian University, Munich, Germany, the Weil Foot and Ankle Institute, Des Plaines, Illinois, University Schleswig Holstein, Campus Lübeck, Lübeck,Germany, the Department of Podiatry, The Permanente Medical Group Inc, Union City,California, the Department of Orthopedics, University Rostock, Rostock, Germany, and the Institute of Sportsmedicine, Frankfurt am Main, Germany
Background: Radial extracorporeal shock wave therapy is an effective treatment for chronic plantar fasciitis that can be administered to outpatients without anesthesia but has not yet been evaluated in controlled trials.
Hypothesis: There is no difference in effectiveness between radial extracorporeal shock wave therapy and placebo in the treatment of chronic plantar fasciitis.
Study Design: Randomized, controlled trial; Level of evidence, 1.
Methods: Three interventions of radial extracorporeal shock wave therapy (0.16 mJ/mm2; 2000 impulses) compared with placebo were studied in 245 patients with chronic plantar fasciitis. Primary endpoints were changes in visual analog scale composite score from baseline to 12 weeks’ follow-up, overall success rates, and success rates of the single visual analog scale scores (heel pain at first steps in the morning, during daily activities, during standardized pressure force). Secondary endpoints were single changes in visual analog scale scores, success rates, Roles and Maudsley score, SF-36, and patients’ and investigators’ global judgment of effectiveness 12 weeks and 12 months after extracorporeal shock wave therapy.
Results: Radial extracorporeal shock wave therapy proved significantly superior to placebo with a reduction of the visual analog scale composite score of 72.1% compared with 44.7% (P = .0220), and an overall success rate of 61.0% compared with 42.2% in the placebo group (P = .0020) at 12 weeks. Superiority was even more pronounced at 12 months, and all secondary outcome measures supported radial extracorporeal shock wave therapy to be significantly superior to placebo (P < .025, 1- sided). No relevant side effects were observed.
Conclusion: Radial extracorporeal shock wave therapy significantly improves pain, function, and quality of life compared with placebo in patients with recalcitrant plantar fasciitis.
Keywords: heel pain; plantar fasciitis; shock wave; lithotripsy; radial extracorporeal shock wave therapy
The American Journal of Sports Medicine, Vol. X, No. X
Orthopedic trigger point shock wave therapy with focused and radial shock waves: a review of the current situation
Orthopedic Surgery, Dr. Gleitz, Luxemburg Introduction
Myofascial pain syndromes are among the most frequent orthopedic disorders. However, efforts to treat these syndromes often show limited success. This is confirmed by the multitude of competing therapy options available today.
According to the theory established by Travell and Simons in their Trigger Point Manual (1992), muscular trigger points are one of the main causes of myofascial pain. Clinical observations and experimental examinations conducted by Travell and Simons have corroborated this theory, demonstrating that muscular trigger points cause diverse functional disorders. These findings coincide with the information provided by patients on pain development and progression. Despite the impressively detailed description of muscle- associated pain syndromes in the Trigger Point Manual (1992), trigger point therapy is still only rarely used in orthopedic practice.
The role of trigger points in causing pain and discomfort is evidenced by the clinical symptoms they may generate: formation of muscle knots with local and referred pain, muscular taut bands, twitch response, reduced range of motion (ROM) of joints, formation of satellite trigger points, development of pseudoradicular dysesthesia and vegetative accompanying reactions.
According to Simons' "integrated hypothesis of trigger point formation" (1996), trigger points are produced by muscular motor end-plate dysfunction which may be caused by various mechanisms, such as acute mechanical overstrain, including trauma, chronic overstrain caused by monotony of motion (repetitive strain injury), poor posture, cold, emotional distress, or result from articular, neurogenic, visceral, hormonal or remote muscular disorders.
The increased calcium release resulting from the above lesions causes a permanent contracture of the actin/myosin filaments (abnormally contracted sarcomeres) under the dysfunctional end-plate and thus leads to increased energy consumption. At the same time, the capillary compression caused by the contraction knots produces local ischemia. The concurrence of these two factors causes a local energy crisis. Local ischemia induces the release of bradykinine in the tissue and of other substances sensitizing muscle nociceptors and increases the tenderness to pressure of the trigger points (allodynia, hyperalgesia). Ischemia causes additional motor end-plate dysfunction and thus creates a vicious circle. Muscles affected by trigger points exhibit changed properties. Apart from the typical contractures, these muscles are characterized by a reduced development of muscular force, delayed relaxation after activity, tendency to spasm and decreased fine motor skills (coordination). These conditions explain the muscles' susceptibility to additional lesions (muscle strain, torn fibers, etc.).
Trigger points cause alterations in the nervous system that contribute to the chronification of pain. These alterations include peripheral sensitization of muscle nociceptors, increased number of nociceptors, activation of the axon reflex, central sensitization (synaptic transmission) and failure of inhibiting interneurons of the supraspinal descending antinociceptive system (8).
If trigger points continue to exist over a prolonged period of time, they may activate satellite trigger points in other muscles. These satellite trigger points will develop their own pain patterns and functional disorders. This will eventually induce myopathic chain reactions (2) with complex pain patterns and secondary structural alterations in the form of insertional tendinopathies (3).
The typical referred pain caused by trigger points is explained on the basis of the "convergence projection theory" (13). This theory postulates that the information from diverse peripheral receptors in various tissue regions is centrally transmitted through a common segmental dorsal horn neuron, which causes a misperception of pain in the patient. If doctors use an approach that is entirely based on classical neurological innervation patterns, this phenomenon makes it extremely difficult to localize the pain origin.
Muscular trigger points require specific treatment owing to their low self-healing capacity. One of the most effective therapy procedures is the application of strong mechanical pressure to the muscle knots (gelotripsy) followed by muscle stretching (17). The following reasons for the efficacy of this therapy approach are discussed: resolution of permanent actin/myosin contractures, improvement of local circulation (reactive hyperemia) along with the elimination of the ischemia-induced energy crisis (8) and reduction in the concentration of vasoneuroactive substances.
Summary
Key words: ESWT – trigger points – myofascial pain syndrome
Orthopedic trigger point shock wave therapy with focused and radial shock waves
The trigger point therapy of Travell and Simons is the starting point for the diagnosis and treatment of myofascial pain syndromes. As trigger points are difficult to localize and trigger point therapy has only limited efficiency, this therapy option is rarely used in practice.
Shock wave application to trigger points represents a new therapy approach in trigger point treatment. The combined use of radial and focused shock waves allows effective local trigger point treatment as well as shock wave application to a wider muscle surface area. Focused shock waves can be used to induce referred pain for precise trigger point localization.
The experience gathered by the authors has shown that a wide range of functional disorders can be treated with trigger point shock wave therapy. The therapy success is based on recognizing muscular trigger points as the origin of pain, which sets this therapy apart from conventional treatment methods.
No scientific evidence is available to date explaining the precise mode of action of shock waves applied to muscular trigger points.
Trigger point shock wave therapy
Application of shock waves to muscles
Since the mid-1990s, various publications have discussed the possibility of muscle treatment with low-energy focused shock waves (4, 5, 7, 14) as an alternative to manual therapy. The common result of the treatments conducted is a reduction of muscle tone along with a diminished extent of muscle shortening.
Since the late 1990s, muscular trigger points have also been treated with radial shock waves (rESWT) with a tissue penetration depth of 20 to 25 mm. While no scientific evidence is available to date explaining the exact mechanism of radial shock waves, extensive molecular and biochemical research has been conducted into the mode of action of focused shock waves (6, 18). In fact, focused shock waves induce a reduction of nociceptive fibers, whereas radial shock waves seem to have a counter-irritation and pain modulating effect through GABAergic interneurons in the dorsal horn. In addition to this action, the pressure and vibrations of radial shock waves improve blood circulation and lymphatic drainage.
Indications and contraindications
Trigger point shock wave therapy can be used to treat all acute and chronic myofascial disorders, provided that no primary disease is present that causes the muscular trigger points and prevents their elimination. In the latter case, trigger points and entire trigger point chains must be seen as part of complex disease patterns such as visceral and psychic diseases, craniomandibular dysfunctions or foot deformations with proprioceptive control disorders. Such conditions should be treated by conducting a causal therapy of the primary disease on the one hand and by eliminating the trigger point syndromes on the other hand. Trigger point therapy is most successful if the primary disease causing the trigger point symptoms can be entirely cured or if its intensity can at least be minimized. Despite causal therapy, trigger points are frequently found to persist or to develop independently. This condition, which is referred to as autonomous trigger point syndrome, can be well treated with trigger point shock wave therapy.
One example for this phenomenon is pseudosciatica after successful discectomy. The trigger points in the gluteal muscles, external rotators (e.g. piriformis muscle) and quadratus lumborum muscle that were activated by the original nerve compression continue to persist despite the fact that the root compression has been eliminated. Successful resolution of these trigger points is only possible by means of trigger point therapy.
Examples of poor indications for trigger point therapy are genuine radicular lesions or advanced spinal or foraminal stenosis in the lower lumbar segments, also with secondary trigger points in the gluteal or hip muscles. Although trigger point therapy of these conditions frequently provides alleviation of pain, this effect will only be of short duration owing to the dominant nature of the nerve compression.
Trigger point therapy is not successful in the treatment of the following disorders: all types of rheumatism with inflammatory activity, severe fibromyalgia and severe vegetative dystonia. General contraindications for trigger point therapy include malignant tumors, primary myopathies, serious rheumatic diseases (e.g. rheumatic polymyalgia) or treatment areas above vulnerable structures. During shock wave therapy, it is crucial that pulmonary tissue is not within the target area of focused shock waves. Relative contraindications include pregnancy and anticoagulant therapy.
Radial or focused shock waves?
The combined use of focused and radial shock waves is one of the recent developments in trigger point therapy. With this approach, focused shock waves are used to treat both tendon insertions and muscles.
The application of focused shock waves to tendon insertions is recommended whenever muscle shortening caused by trigger points has resulted in secondary insertional tendinopathies. In these cases, treatment of the muscular trigger points alone would not be sufficient to cure the disease as the tendon irritation is often responsible for the dominant pain symptoms and would persist as an independent cause of pain even after successful muscular trigger point therapy.
Focused shock waves applied to muscles are used for diagnostic and therapeutic purposes. On the one hand, they ensure precise localization of the trigger points as the typical referred pain can be induced more reliably than during manual examination. On the other hand, focused shock waves are used for the local treatment of individual trigger points. Thanks to the minimal irritation they cause, focused shock waves can also be used for the trigger point therapy of extremely painful muscles.
Radial shock waves are used for the local treatment of muscular trigger point areas and, subsequently, for smoothing the residual muscle. This method allows large muscle regions to be treated with radial shock waves.
When treating extremely painful myofascial syndromes, only focused shock waves should be used during the initial therapy sessions. Treatment can then be continued with radial shock waves at low therapy pressure (1.6 – 1.8 bar). Promising experience has been gathered recently in the use of defocused shock waves for the treatment of trigger points or insertional tendinopathies. "Defocused" means that the generated waves are applied to the tissue not in a single spot but over a wider surface area.
Therapy planning
The muscles to be treated are selected on the basis of the following criteria: patient's indication of pain, diagnosis of muscle knots (manually or with radial shock waves), possible provocation of referred pain by palpation pressure or with focused shock waves and, where possible, ROM testing to identify the muscles affected by reductions in the range of motion. The anamnesis and description of the pain with respect to the pain location and referral are of special importance. Detailed knowledge of muscle-specific pain patterns, which deviate entirely from classical neurological innervation patterns, allows early identification of the muscles involved in the pain syndromes. Descriptions of pain provided by patients, which do not make sense under neurological aspects, prove astonishingly coherent and informative when considered under trigger point aspects, all the more so because trigger points can also be responsible for dysesthesia, coordination disorders and loss of strength.
Knowledge of the muscle-specific pain referral described by Travell and Simons (1992) represents an indispensable requirement for every therapist. Increasing experience in trigger point therapy, especially in the use of focused shock waves, has shown that pain referral patterns and the location of muscle knots vary in each patient and need to be identified by accurate examination.
Localization of trigger points
The induced referred pain is a major criterion for the selection of the therapy region. Strong manual pressure is exerted on the muscle knots to cause referred pain. Focused shock waves can be applied to induce referred pain more easily and accurately. Depending on the muscle thickness and depth of the trigger point areas, focused shock waves with variable penetration depth are applied at an energy level of between 0.05 and 0.25 mJ/mm2.
Radial shock waves are less suitable for the localization of trigger points on the basis of referred pain. Radial shock waves are rather used to identify indurations inside the muscles. This is done by moving the applicator over a large muscle area during the therapy.
Therapy procedure
The trigger points to be treated are selected according to the criteria of short-term or long- term reduction of the pain symptoms. Therapy is started by treating the active trigger points which are responsible for spontaneous current pain or pain on exertion.
This is followed by the treatment of satellite trigger points in the area of pain referral. Similarly to secondary trigger points in the functional muscle chains of antagonists and synergists, satellite trigger points are responsible for the chronification process if they persist for a prolonged period of time.
Insertional tendonitis, which Travell and Simons (1992) describe as peripheral trigger points, should be given special attention. These trigger points must be treated with focused shock waves. However, contrary to the treatment of muscular trigger points, a reduction in pain is only perceived several weeks after the therapy. This is due to the slowness of the induced physiological repair mechanisms. In this context, the energy flux density is of major importance. Experience has shown that shock waves should be applied at a low energy level in order not to affect the cell recovery potential, that is the useful neurogenic immediate tissue response. Since treatment is performed on a biological system, the therapy intervals between the individual sessions should not be too short (at least 1 to 2 weeks) and the number of therapy sessions should be limited. It is also crucial that no local anesthetic be used prior to shock wave application (12).
Accompanying therapies
In principle, no accompanying therapies are required to achieve the desired therapy success. However, shock wave therapy can be supported by trigger point stretching in fiber direction. In the presence of severe joint blockage, the blockage may loosen as a result of muscle relaxation after shock wave therapy. If this is not the case, manual therapy can be performed to eliminate the blockage after the first two or three trigger point therapy sessions and after muscle tension has started to decrease. Additional therapies, such as massaging, should not be used.
Muscle strengthening therapy can be performed one to two days after the trigger point therapy. However, it is crucial that this therapy not be performed with maximum force or at the point of maximum muscle shortening.
In the treatment of chronic pain syndromes, ibuprofen or paracetamol should be administered at the beginning of the trigger point therapy to relieve the pain.
Treatment parameters and duration
The energy flux density of focused shock waves used in muscular trigger point therapy is between 0.05 and 0.25 mJ/mm2. Higher energy levels should not be used to avoid tissue damage (11). Judging by the latest scientific research results, the shock wave frequency applied to the trigger point should not exceed 4 Hz.
The energy flux density (mJ/mm2) is selected on the basis of the thickness and depth of the muscle and the patient's indication of pain during localization of the trigger points and provocation of referred pain. The energy flux density should be selected in such a way that the pain induced by the shock waves can still be well tolerated by the patient. Generally speaking, the energy level can be increased after each therapy session as the pain perceived during shock wave application gradually decreases if the therapy progresses smoothly.
The same applies to radial shock waves. The therapy pressure of radial shock waves varies between 1.6 and 4 bar, depending on the shock transmitter size and the patient's indication of pain. Shock transmitters with a small surface should be used with extreme caution owing to the high peak pressures they may generate. Judging by our experience, such shock transmitters are generally not required for the muscles to be treated. The pressure applied should be adequate for the tissue properties to avoid hematomas. The shock wave frequency is 10 to 15 Hz, where the 15 Hz frequency is generally perceived as causing less pain. This effect may be attributable to the physiological intrinsic muscle oscillation stimulated by the radial shock waves.
In the combined use of focused and radial shock waves in trigger point therapy, the trigger points are first treated locally, applying 200 to 400 focused shock waves. This step is followed by muscle smoothing of the agonists, antagonists and synergists with the radial shock wave transmitter, applying 3000 to 4000 radial shock waves. If muscles are treated with radial shock waves alone, the trigger point area is treated locally with 500 to 1000 shock waves and without applying manual pressure. This step is then followed by muscle smoothing with up to 4000 shock waves at a frequency of 15 Hz, in accordance with the stretch-and-spray technique developed by Travell and Simons (1992).
Treatment frequency
A therapy frequency of one session per week has shown to be ideal for most patients. These intervals enable the muscles to recover from the irritation, which may initially persist for up to three days. Shorter intervals might cause additional muscle irritation before the irritation from the previous session has actually disappeared and thus increase pain. Insertional tendonitis should not be treated at shorter intervals in order not to affect the aforementioned regeneration potential that results from the local neurogenic tissue response. Pain modulation aspects, too, suggest that the treatment intervals in trigger point shock wave therapy, similarly to acupuncture, should not be too short. The following general principle applies: longer therapy intervals and lower treatment intensities should be used for more serious and chronic pain syndromes.
Therapy progress: pain relief, side effects and complications
In the treatment of most trigger point syndromes, a reduction in pain is generally perceived after 4 to 6 therapy sessions, or even after as little as 1 to 2 sessions in the case of short- term conditions. Chronic syndromes with many different affected muscles require 6 to 10 or even more therapy sessions to eliminate the pain. If the therapy proves unsuccessful after this many sessions, treatment should be interrupted and the indication should be checked.
A short-term increase in the original pain and, in very rare cases, the manifestation of other muscular disorders may occur after the initial sessions. Shock wave application to the cervical spine may cause headache and temporary buzzing in the ears, especially when radial shock waves are used. Patients who are suffering from migraine or are susceptible to tinnitus must be informed about these possible side effects. In these cases, the shock waves should be applied at a low pressure (1.6 bar), and patients should wear ear protection. The same applies to the application of focused shock waves.
No serious complications will occur if the shock waves are applied correctly in terms of the shock wave energy levels and penetration depth. The most frequent side effects include local hematomas, especially in the gluteal muscles, caused by radial shock waves.
Should a temporary interruption of the therapy prove necessary due to the aggravation of pain or the extent of the hematoma, the therapy intensity (energy flux density, treatment pressure and total number of shock waves applied) should be reduced when treatment is continued. The intensity can then be increased again during the following therapy sessions.
Therapy success
Trigger point shock wave treatment is considered successful if over 80 % of the original pain has been eliminated at the end of the therapy. The residual 20 % may well disappear during the three months following the therapy, which means that it does not make sense to permanently continue treatment. A successful therapy should provide lasting pain relief or at least eliminate the pain for 6 to 12 months.
If the original pain is reduced by as little as 50 %, additional trigger points are likely to exist in the functional muscle chain. These trigger points, which may be latent in nature, should be identified. If pain reduction rates of only 20 to 30 % are achieved at the end of the therapy or if the pain relief lasts only a few weeks, additional differential diagnostics of the disorder will be necessary.
Orthopedic disorders with high SockwaveTherapy success rates
The recommendations below are based on several years of experience acquired by the authors in the field of orthopedic trigger point shock wave therapy.
Cervicalgia, cervical cephalalgia, cervicobrachialgia
These indications respond particularly well to trigger point shock wave therapy as the affected muscles (except for the trapezius muscle) are rather small and located close to the body surface. The local pain, which climbs up into the head, is primarily caused by the descending and horizontal parts of the trapezius muscle and by the semispinalis muscle, splenius muscle, levator scapulae muscle and sternocleidomastoideus muscle. Apart from the scaleni muscles, the muscles that are responsible for pseudoradicular brachialgia are all located in the shoulder girdle region (subscapularis muscle, infraspinatus muscle, teres muscles, serratus posterior superior muscle, pectoralis muscle). A reduction in pain is achieved after 6 to 8 therapy sessions, along with a lasting increase in mobility of about 20 degrees rotation, 17 degrees inclination/reclination and 17 degrees lateral inclination. If no improvement is achieved, examinations should be conducted to find out whether the patient suffers from temporomandibular dysfunctions or psychovegetative exhaustion.
Lumbalgia, pseudoradicular lumbosciatica
These indications can also be treated successfully, provided that the patient does not suffer from dominant radicular irritations (prolaps, foraminal stenosis with segmental deficiencies), arthrogenic irritations (activated facet syndrome, spondylolysis) or discogenic irritations (erosive discopathy). Local pain in the lumbar spine is caused by trigger points in the segmental muscles (multifidi and rotator muscles), in the dorsolumbar junction (iliocostalis lumborum and thoracis muscle) and in the iliopsoas muscle. Referred pseudoradicular pain is caused by trigger points in the gluteal muscles (gluteus minimus and medius muscles), in the external hip rotators and in the quadratus lumborum muscle. In these cases, referred pain (in the lower leg and foot) can be easily induced by applying focused shock waves.
Dorsalgia
The primarily local pain is caused by trigger points in the multifidi and rotator muscles and, in the interscapular region, by trigger points in the rhomboidei muscles, serratus posterior superior muscle and in the ascending part of the trapezius muscle.
Periarticular shoulder pain and restricted mobility
The term "periarthritis", often reluctantly used, plays a major role in the description of these conditions as many types of shoulder pain originate in the periarticular muscles and cause restricted mobility (infraspinatus muscle with reduced internal rotation and anterior shoulder pain, subscapularis muscle with reduced external rotation and posterior shoulder pain). Referred pain in the lateral upper arm is caused by trigger points in the horizontal part of the trapezius muscle, in the supraspinatus muscle and in the deltoid muscle. Insertional inflammations of the supraspinatus tendon have to be treated separately with focused shock waves. Frozen shoulder, a condition characterized by painful shoulder stiffness and pain caused by capsular contracture, cannot be treated successfully with trigger point shock wave therapy.
Radial and ulnar epicondylopathy
In general, these indications are no promising candidates for trigger point therapy. Most disorders are caused by local insertional tendinopathy, and not by referred pain. However, early stages of these conditions, which are caused by muscular overstrain of the forearm flexor and extensor muscles, can be treated successfully. In the case of chronic pain syndromes, treatment of the muscle chains is a viable attempt. Radial epicondylopathy: scaleni muscles, horizontal part of trapezius muscle, supraspinatus muscle, lateral part of triceps brachii muscle, anconeus muscle, supinator muscle, brachioradialis muscle including forearm extensor muscles. Ulnar epicondylopathy: serratus posterior superior muscle, infraspinatus muscle, pectoralis muscle, medial part of triceps brachii muscle, pronator teres muscle and forearm flexor muscles. Local insertional tendinopathies have to be treated with focused shock waves.
Wrist tendonitis
Wrist tendonitis is caused by overstrain of the forearm muscles involved in wrist movement. Accompanying trigger point shock wave therapy must be performed by applying shock waves to the affected forearm muscles.
Pelvic/hip pain
Pelvic/hip pain can be successfully treated with trigger point shock wave therapy. The frequently diagnosed trochanteric bursitis is often caused by trigger points in the gluteal muscles and the external hip rotators. Local trochanteric pain has to be treated with focused shock waves. These trigger points may have been caused by previous lumbar spine pain syndromes or by a developing coxarthrosis and residual conditions after total endoprosthetic surgery. Sciatic pain, which is caused by trigger points in the gluteus maximus muscle and in the ischiocrural muscles, responds well to trigger point shock wave therapy.
Tensor fasciae latae syndrome
Overstrain of the tensor fasciae latae muscle is very common among runners and causes lateral hip and thigh pain. This condition is often accompanied by trigger points in the gluteal muscles and vastus lateralis muscle.
Adductor tendinopathies
Although adductor muscles can be easily reached with shock waves, they are still difficult to treat. This is due to the fact that, in addition to trigger points, there are insertional tendinopathies in the proximal and medial third of the muscles on the pelvic insertion.
Shortening of thigh flexor and extensor muscles
The most frequent symptom of this condition is recurrent muscle sprain caused by increased muscle tension. It can be treated successfully with shock wave therapy, but requires a high number of shock waves due to the large size of the muscles involved.
Patellar chondropathy
This condition is often characterized by a shortened quadriceps and by trigger points in the medial and lateral vastus muscles near the knee joint. Quadriceps shortening can be reliably objectivated by measuring the heel-to-buttock distance in prone position. Successful results are achieved after only two to four therapy sessions. Moreover, parapatellar pain often manifests itself after total endoprosthetic surgery and can be well treated with trigger point shock wave therapy.
Patellar tendonitis
In addition to the symptomatic tendonitis, which can be treated locally with focused shock waves, this condition is often characterized by a shortened quadriceps muscle. Although trigger point shock wave therapy provides excellent quadriceps relaxation, the tendonitis often takes several months to cure completely.
Shin splint
Tendons and the periosteum are the dominant pathological features of shin splints and must be treated with focused shock waves. Accompanying radial shock wave therapy can be performed to eliminate indurations in the medial calf muscles and in the flexor hallucis longus muscle.
Anterior tibial syndrome
Trigger point irritation of the anterior tibial muscle is encountered among runners and after mountain descents due to muscular overstrain. Shock waves are exclusively applied to the muscles.
Achillodynia
The dominant pain symptoms in achillodynia are caused by tendonitis, which is treated locally with focused shock waves. Achillodynia is frequently accompanied by calf muscle shortening. Shock wave therapy should be extended to treat these contractures as a reduction in the calf muscle tension by trigger point therapy will also relieve the Achilles tendon (similarly to raising the heel) and is reported by patients to provide rapid alleviation of pain. The experience gathered by the authors has shown that trigger point therapy ensures a lasting improvement in the frequently restricted active ankle joint extension from 16 degrees to 25 degrees after 4 to 5 sessions.
Plantar fasciitis of the heel (plantar calcaneal spur)
In most cases, sonographic diagnosis reveals that the frequent X-ray diagnosed calcaneal spur is a severe plantar fasciitis below the calcaneus, characterized by fascial swelling of 4.5 to over 12 mm (normal value < 4.0 mm). This means that on the one hand local therapy is required, applying focused shock waves to below the calcaneus. On the other hand, the therapy should also focus on eliminating muscle contractures of the calf muscles and plantar muscles, which form a functional chain.
Metatarsalgia
Pain in the forefoot is frequently caused by splay foot related overstrain of the longitudinal and transverse muscles. This pain can be reliably eliminated with radial shock waves in 4 to 5 sessions, provided that it is not accompanied by periosteal irritations of the metatarsals and that Morton's neuromas are excluded.
Discussion
The many different types of disorders described above have shown that the combination therapy with focused and radial shock waves can be successfully used for a variety of indications in the treatment of myofascial pain syndromes. It has been pointed out that an accurate anamnesis, especially with respect to the patient's indication of pain, is of special importance. Extensive differential diagnostics is, of course, required, which means that extracorporeal shock wave therapy is and will continue to be a medical procedure to be performed by doctors. Even if radial shock wave therapy is delegated to a physiotherapist, the diagnosis must still be made by the physician. If no lasting improvement in the condition is achieved or in case of a poor therapy success, the physician will be required to re-examine the patient.
Palpation or pinch test diagnosis with provocation of the typical referred pain and local twitch response of the muscle, which is sometimes impossible to induce, continue to play a major role in clinical screening. Functional and stretching tests are performed to complement clinical examinations. The use of focused shock waves for the localization of muscular trigger points has proved its worth as a new diagnostic procedure. This method is more accurate than localization by dry needling. The characteristic referred pain can be reliably induced. Pain localization with focused shock waves is performed at a low frequency (3 Hz) to ensure successful feedback from the patient. Treatment is started after having successfully localized primary, satellite or secondary trigger points.
The precise mode of action of shock waves applied to muscular trigger points has not been defined to date. However, the shock wave mechanism can be explained on the basis of known theories (1).
The pain relief provided by shock waves is due to counter-irritation and pain modulation comparable to dry needling. Owing to the specific physical properties of shock waves, this therapy can be described as needle-free acupuncture which induces a down-regulation of nociceptive afferents through enkephalinergic interneurons in the dorsal horn of the spinal cord. The pain modulation achieved with radial shock waves through the activation of A-beta fibers in the muscle, which then provide pain inhibition through GABAergic interneurons in the dorsal horn, can be explained in a similar manner. This would confirm the findings of Travell and Rinzler (1952), who observed many years ago that pain is relieved and trigger points are eliminated after pressure and stretching. The vibration (15 Hz) of radial shock waves also seems to have a favorable effect on muscular structures. The physiological intrinsic oscillations of 15 to 30 Hz have been described by Nazarov (1988) as important for muscular blood circulation and lymphatic drainage.
On the basis of Simons' integrated hypothesis of trigger point formation (1996), according to which muscular end-plate dysfunction and an energy crisis caused by local ischemia are the central features of trigger point pathologies, the following additional shock wave mechanisms are discussed: mechanical resolution of permanent actin/myosin contractures through local transverse stretching of the sarcomeres by the application of shock waves perpendicular to the fiber orientation up to the destruction of abnormally contracted sarcomeres through the energy applied, reactive local tissue hyperperfusion and angioneogenesis (18), which would eliminate the ischemia responsible for the energy crisis, and eventually thinning of vasoneuroactive substances by the pressure exerted on the tissue by shock waves. All these mechanisms could explain the clinically observed reduction in muscle tension and muscular contracture.
Judging by the results of recently conducted animal tests, the effects of focused shock waves in the treatment of insertional tendinopathies, referred to as "attached trigger points" by Travell, are molecular, biochemical and cellular in nature (6, 10). Neurogenic messenger substances such as substance P or CGRP are considered to induce plasma extravasation, angiogenesis and neurogenic inflammation. Similarly to the chemical stimulus produced by capsaicin, shock waves used to induce a mechanical stimulus can cause immediate local tissue response, which would explain the regeneration of tendon tissue.
While the results of the aforementioned animal tests and pain therapy considerations may explain the effects of extracorporeal shock wave therapy in the treatment of trigger point syndromes associated with insertional tendinopathies, no clinical confirmatory studies have been conducted to date to verify the experience gathered in practical application. Further research is therefore required by university scientists and by the shock wave study group of the DGOOC (German Society for Orthopedics and Orthopedic Surgery).
Authors' contact address:
Dr. med. M. Gleitz
Orthopädische Praxis
[Orthopedic Surgery]
30, Grand Rue
L-1660 Luxembourg
E-mail: marklux@mail.anonymizer.com

